Why do I say we do not need the new norm but instead needs a strong and very efficient state of the art public health system? Let me explain in a way an Engineer like me would think. A reminder to the reader: This my own “takes” in fighting COD-19 disease that is ‘scourging’ our Country today.
Engineers sees a problem as a system. Also, Engineers follow Peter Ducker’s Principle– “You cannot manage what you cannot measure”.
Since March 18, 2020 at the start of the Enhance Community Quarantine (ECQ} I took notes of the following information from the Department of Health (DOH), Number of Persons with COVID-19 Infections (A), Number of Deaths (B) and Number of Recoveries (C). It took me sometime to analyze the data until I learn from the news that 17 doctors have died of COVID-19 infection. Being familiar with the ASHRAE 170 Standard for Healthcare Facilities I knew that there are no standards for an area of refuge for healthcare personnel in hospitals. I emailed the American Society of Heating Refrigeration Airconditioning Engineers (ASHRAE) of my concern and proposed a standard for an area of refuge for healthcare personnel in hospitals which they agree to study and eventually urge me to be a volunteer of the SSP-170 Healthcare Standards Committee. I accepted the offer. I made a request for the interpretation of some sections in ASHRAE 170 especially the term “asepsis”. I got hold of the medical protocol “asepsis” thru the National Nursing Org. Standards. I learn that “asepsis” is a medical protocol of healthcare personnel with two procedures namely the medical asepsis and the surgical asepsis. But part of the protocol in hospitals is “to prevent airborne transmission of diseases” is the job of design engineers.
After my engagement with ASHRAE I took interest to the DOH COVID-19 data. I found that the three data released by DOH, with reference to mathematics, are all independent variables. This means no interpretation can be extracted except as collation of information and not for analysis. After a day looking at the DOH data, I knew I will need a data that is dependent from one independent value or variable that would describe a system. From the data tabulated below, columns “A”, “B” and “C” are the number of persons recorded daily by DOH. These are independent values which has no mathematical relationship with each other. The accuracy of this figures relies on DOH tabulators.
What I did to create a dependent value or variable by adding column “B” and column “C” and sum of these two columns is subtracted from column “A’ giving us a dependent value in column [A – (B+C)] = D which is an accurate representation of the confirmed cases infected daily in present value. Column “D” now a dependent value to two independent values in columns “B” and “C”. Columns “B” represents the number of deaths while column “C” represents the number of recoveries which I consider as a measure of efficiency of our public health system to successfully handle any pandemic disease that enters our Country. Please refer to the Table1.0 below:
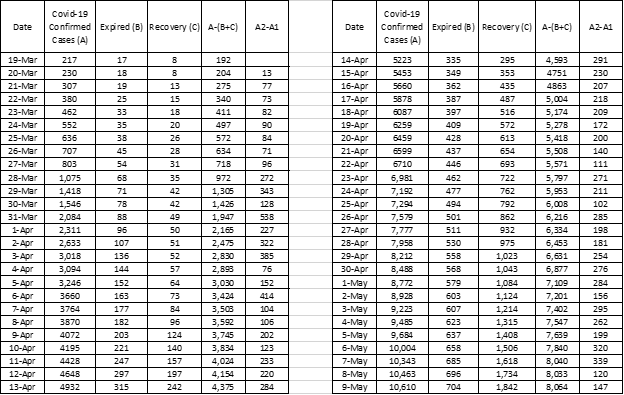
To elaborate further, when the number of deaths is higher than the number of recovered persons it means our public health system is not able to handle pandemic situations. If the number of recoveries is equal to the number of deaths, the public health system is a failure. When the number of recoveries is more than the number of deaths the public health is average. I categorize the public health system into five levels as shown below in Table 1.0
| Description of Category | Public Health System Performance | Remarks | |
| 1 | Number of Deaths is Greater than the Number of Recoveries | Poorly Ineffective | Curve is Linear (Up) |
| 2 | Number of Deaths is Equal to the Number of Recoveries | Ineffective | Curve is Linear (Up) |
| 3 | Number of Recoveries is Greater than the Number of Deaths | Satisfactory but Ineffective | Curve is Linear (Up) |
| 4 | Number of Recoveries is Equal to the Number of Column “D” or [A – (B+C)] | Good Needs New Normal | Needs Curving Down of Curve |
| 5 | Number of Recoveries is Equal to the Number of Infections Column “A” | Excellent No Need for New Normal | Curving Down the Curve is Automatic |
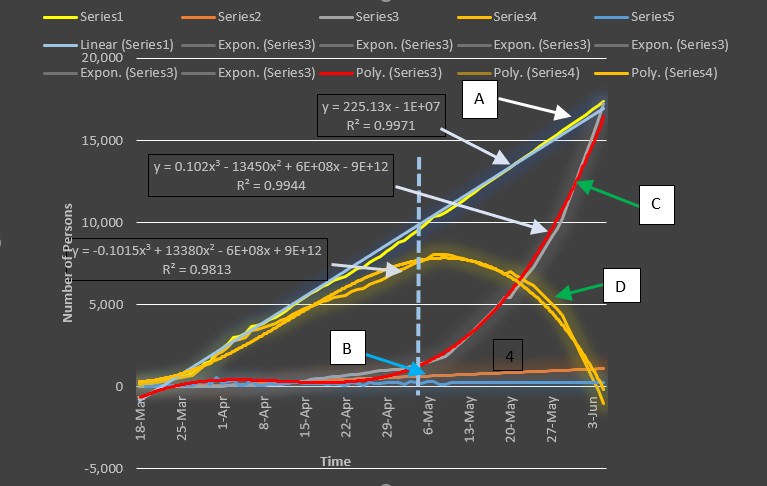
In Chart 1.0 below shows the present performance levels of the of the public health system versus COVID-19. The box in Table 1.0 represents performance of the public health today. Beyond the vertical blue dash line are forecasted based on assumed data in Table 2.0. The box

represents Category 4 in Table 1.0 where the number of recoveries is equal to the number of infected persons. This Category represents the intersection as shown in Chart 1.0 which happens ideally when the number of recoveries is forecasted to be as in Table 2.0 below:
| Number of Recoveries Per Day | Forecasted Dates | Every Number of Days |
| 375 | May 14 to May 18, 2020 | 5 |
| 450 | May 19 to May 23, 2020 | 5 |
| 600 | May 24 to May 28, 2020 | 5 |
| 1000 | May 29 to June 05, 2020 | 9 |
At Category 4 the curve “D” (yellow) in the Chart 2.0 below curved down to box . but will not drop to zero because curve “A” continuously rises at 250 infected persons per day and is vulnerable to sudden spike of curve “A”. To be invulnerable, the number of recoveries should increase to 600 persons per day to 1,000 persons per day. This is the heart of my conclusion that- Can our public health system be able to increase the number of recoveries to 1000 persons per day at 250 persons infected per day. This Is the question that the government should address to place COVID-19 to a level as Dengue. At least recovery should be 5 to 11 days without deaths. A similar situation in Taiwan –Republic of China.
“Taiwan is an island of resilience. Centuries of hardship have compelled our society to cope, adapt, and survive trying circumstances. We have found ways to persevere through difficult times together as a nation, and the COVID-19 pandemic is no different. Despite the virus’s highly infectious nature and our proximity to its source, we have prevented a major outbreak. As of April 14, we have had fewer than 400 confirmed cases.” [As of today 440 confirmed cases and 7 dead] Tsalin-Wen of Nhu Xuan Hua for TIME Report on Taiwan’s (Republic of China) fight against COVID-19 :
This brings us to define a public health system. Center for Disease Control and Protection (CDC.gov) defines Public health systems are commonly defined as “all public, private, and voluntary entities that contribute to the delivery of essential public health services within a jurisdiction.” Or as shown I Figure 1.0

There are 10 Essential Public Health Services describe the public health activities that all communities should undertake by CDC.gov:
- Monitor health status to identify and solve community health problems
- Diagnose and investigate health problems and health hazards in the community
- Inform, educate, and empower people about health issues
- Mobilize community partnerships and action to identify and solve health problems
- Develop policies and plans that support individual and community health efforts
- Enforce laws and regulations that protect health and ensure safety
- Link people to needed personal health services and assure the provision of health care when otherwise unavailable
- Assure competent public and personal health care workforce
- Evaluate effectiveness, accessibility, and quality of personal and population-based health services
- Research for new insights and innovative solutions to health problems
In Figure 1.0 the next greatest number of “spokes” is the Neighborhood Organization or our Barangay. Even the 10 Essential Public Health refers this to “communities”. The Barangay “spokes” directly points to: Hospitals, Emergency Medical Service (EMS), Doctors, Community Health Center (CHC), Nursing Homes, Laboratories, Non-Profit Organizations, Home Health and Drug Treatment.
Tsalin-Wen of Nhu Xuan Hua for TIME Report on Taiwan’s (Republic of China) fight against COVID-19 :
“This success is no coincidence. A combination of efforts by medical professionals, government, private sector and society-at-large have armored our country’s defenses. The painful lessons of the 2003 SARS outbreak, which left Taiwan scarred with the loss of dozens of lives, put our government and people on high alert early on. Last December, when indications of a contagious new respiratory illness began to appear in China, we began monitoring incoming passengers from Wuhan. In January, we established the Central Epidemic Command Center to handle prevention measures. We introduced travel restrictions, and established quarantine protocols for high-risk travelers.”
Given this COVID-19 pandemic situation DOH should focus on increasing the capacity of the Hospital ICU beds and medical facilities to include PPE. [These was done in New York and Los Angeles where each 2000 hospital beds were installed including dispatching two US military hospital ships.]. However, it is best that DOH communicate now with the US government to acquire therapeutic drugs[1] to increase the number of recoveries to 1,000 persons per day. There is a COVID-19 vaccine being develop now in the US which can be use in the first quarter of 2021. [ 1 ]
The government should provide efficient Medical Services (EMS) by adding trained doctors and healthcare personnel to work in shifts so that they will not be overwhelm in their work.
[1] Therapeutic Drugs used in the US: Remdesivir, Hydroxychloroquine, Chloroquine, Azitomycin and others. Vaccine will be available on the first month of 2021.
To reduce the number of persons infected by COVID-19 as in Curve “A”, DOH should have a direct hand in conducting 100% testing of COVID-19 at the Barangay level specially the informal settlers. [In Singapore their first weeks had a very few infections but grew to 26,000 persons infected by CVID-19 because the housing facilities of migrant workers was infected. The Singapore government had to transfer ten thousand of migrant worker to military bases.] Similarly, DOH should recommend transferring 75% of the informal settlers to Subic or to Clark before any widespread infection occurs. While the informal settlers are in Subic the government should build descent government building compliant homes in their original abode.
Contact tracing should be made efficient by setting up a national health identification system for all Filipinos.
“Upon the discovery of the first infected person in Taiwan on Jan. 21, we undertook rigorous investigative efforts to track travel and contact history for every patient, helping to isolate and contain the contagion before a mass community outbreak was possible. In addition to the tireless efforts of our public-health professionals, spea rheaded by Health Minister Chen Shih-chung, our informed citizens have done their part. Private businesses, franchises and apartment communities have initiated body-temperature monitoring and disinfection steps that have supplemented government efforts in public spaces.” Tsalin-Wen of Nhu Xuan Hua for TIME Report on Taiwan’s- Republic of China fight against COVID-19:
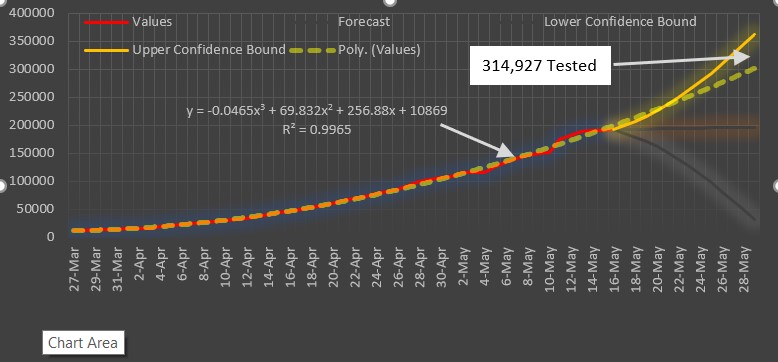
Chart 3.0 forecasted the number of testing of COVID-19 based on the present rate of testing conducted by our government. At least 1.5% of the population should be tested. The US as today tested 2.5% of its population.

Chart 4.0 shows the graph of the Number of Tested Persons since April 15, 2020 which is the start of the increase of testing capacity. Testing should be combined with contact tracing. When a person is tested positive, immediately there after, contact tracing should commence vigorously until all the persons who got in touch of the infected person are tested. This is where a national health identification system become useful. The card should be digitized for fast contact tracing.
Peter Drucker’s Principle– “You cannot manage what you cannot measure”
(My next blog “Why I made this Report?” Also, “Metro Manila Bus Transportation System During COVID-19 Pandemic Situation and Beyond”)

